Continuous Glucose
Monitoring System

What is CGM?
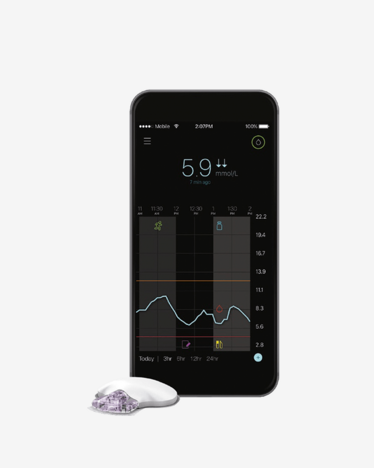
CGM is a Continuous Glucose Monitoring system. It essentially measures glucose levels 24/7, every few minutes, through a tiny sensor. This measures your interstitial glucose level, which is the glucose level found in the fluid between the cells.
Is CGM for me?
Have frequent low glucose levels
Want to reduce HbA1c without increasing hypoglycaemia
Experience fluctuating blood glucose levels

What are the Benefits of CGM?
A CGM system gives you a greater view of your glucose trend
When using Continuous Glucose Monitoring therapy
3 times
more users reached HbA1c level <7.5%2
14.5%
users increased
time spent in range3
A blood glucose meter only provides a brief “snapshot” of your glucose level at a single moment in time. A CGM system gives you a greater view of your glucose trends. CGM can provide valuable information1 at various points during the day, including before and during exercise, prior to driving, before taking an exam or test, and in the middle of the night.
What are the different ways to use CGM?
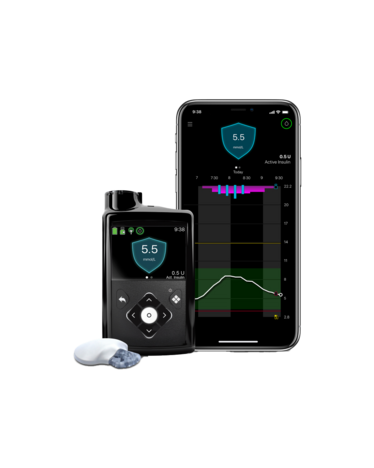
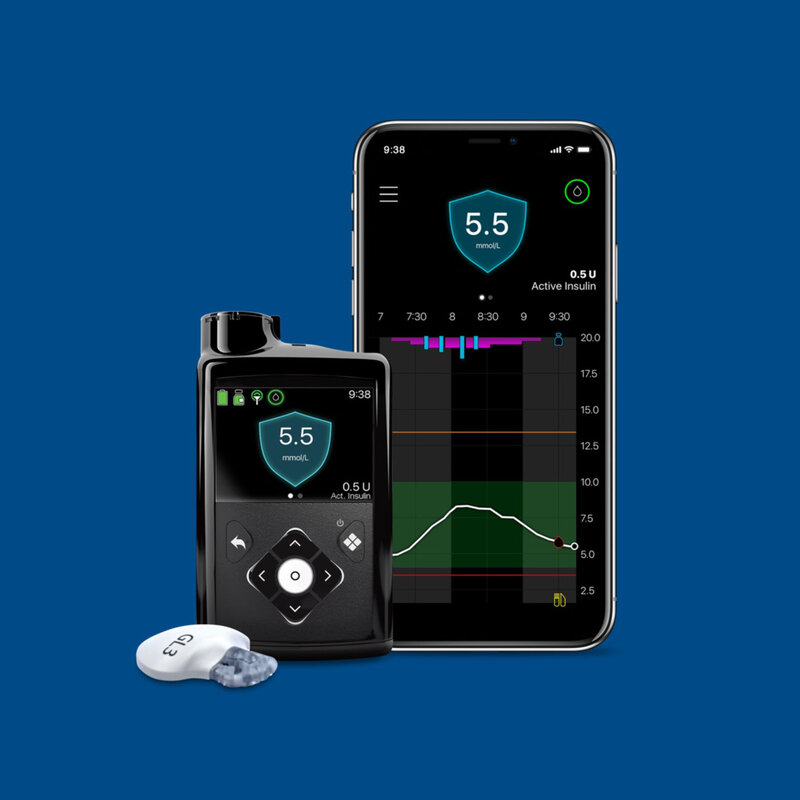
Whether you manage your diabetes with a pump, multiple daily injections, oral medications or through diet and exercise, Medtronic offers CGM products and insulin pump systems that give you, your loved ones and healthcare professionals the insights to track and manage your diabetes on your terms.

Always by your side
We know changing therapy can be daunting at first. Don’t worry, we are here to help you every step of the way.
Whatever you are facing we are always by your side, but not just through creating innovative products. It is also by helping you on your diabetes journey.
With 24/7 online resources and easy to access specialists, we want to empower you with more confidence and comfort in the management of your diabetes therapy.
Know that you are not alone. Know WeCare.
- Rodbard D. DIABETES TECHNOLOGY & THERAPEUTICS 2017;19(3):S25-S37
- Beck RW. et al. JAMA 2017;317(4):371-378.
- Ruedy KJ. et al. J Diabetes Sci Technol. 2017;11(6):1138-1146
- 1.Rodbard D. DIABETES TECHNOLOGY & THERAPEUTICS 2017;19(3):S25-S37
- 2.Beck RW. et al. JAMA 2017;317(4):371-378.
- 3.Ruedy KJ. et al. J Diabetes Sci Technol. 2017;11(6):1138-1146
- *compared to MDI SMBG (multiple daily injection & self monitoring blood glucose)